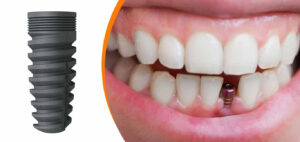
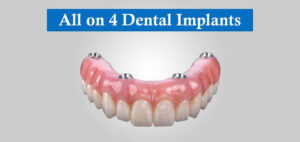
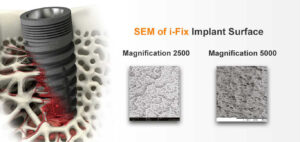
Dental restorative materials, procedures, and strategies that are predictably effective for the long-term management of tooth loss have advanced dramatically. Scientifically validated technologies have evolved to give dental patients with cosmetic and functionally superior tooth replacement solutions. Dental implants have been used to replace lost teeth with a high success rate in a revolutionary fashion for over a century, therefore they were regarded as an important contribution to dentistry.
Today dental implant constitutes one of the most reliable choices for replacing lost teeth. They also help in restoring normal articulation, swallowing, facial attractiveness, and aesthetics to patients around the globe. However, the capacity of the implant material to integrate with the surrounding tissues is critical to its success. Also, several other parameters, including implant material, implant loading condition, and bone quality and quantity influence the integration process. Therefore, understanding of fundamentals of placing dental implant is crucial for its long-term function and success.
Key factors to consider in dental implant placement:
Dental implant placement protocol requires consideration of many factors. Some of which can be patient factors, implant material factors and clinical related factors. One should follow these following steps during dental implant placement:
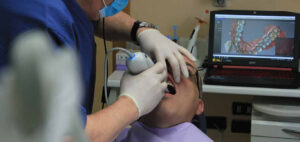
Step-1: Diagnosis and treatment planning:
A proper diagnostic and treatment regimen are critical for the long-term effectiveness of dental implants. Comprehensive medical and dental histories, clinical pictures, study casts, and periapical and panoramic radiographs are basic requirements. Also, with the help of computerized or linear tomography of the intended dental implant placement sites should all be evaluated. Prognosis of the dentition, and in particular the prognosis of the tooth in question, are critical in treatment planning.
The crown-to-root ratio, residual root length, periodontium attachment level, interproximal involvement, and periodontal functional capacity should be looked into. Moreover, considerations should be given to teeth next to the proposed implant location and root fractures with large endodontic posts. Implants are considered as choices of treatment for non-vital teeth and those with roots shorter than 13 mm.